Substance Induced Mood Disorder
All You Need to Know About Substance Induced Mood Disorder
Substance induced mood disorder is a type of depression that is caused due to consumption of drugs, alcohol, or medications. Medication / substance induced depressive disorder is the medical name for alcohol or drug-induced depression.
Overview of SIMD:
The fact about substance induced depression is that most people consume drugs to feel better, however, those same drugs make them feel even worse due to the associated side effects.
When psychologists or doctors give a diagnosis of substance/medication-induced depressive disorder, they perform a complete analysis to make sure that the depression was not there before the consumption of alcohol, medications, or drugs which might be responsible for low mood. This is because there are different types of depressive disorders and if the symptoms of depression were present before the substance use, it is not the substance/medication-induced type of depression/mood disorder.
Following Topics of This Blog Have Been Discussed Below:

Symptoms of Substance Induced Mood Disorder
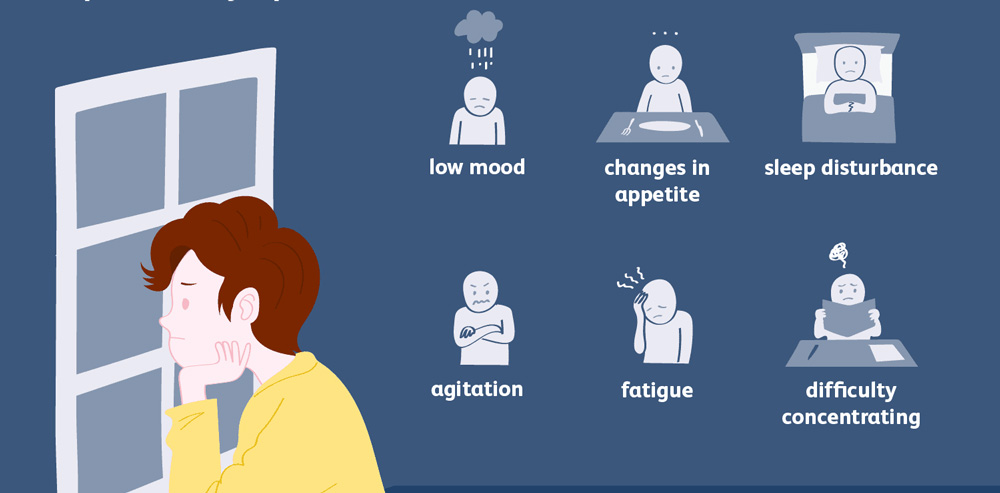
The symptoms of the mood disorder should be severe enough to cause deteriorating effects in the day-to-day functioning of the individual. Withdrawal times for various substances from the body are usually different, and so the depressive symptoms may remain persistent for some time after the individual has stopped the consumption of the substance/medication. Common symptoms are:
- Persistently feeling sad, hopeless, or empty
- Persistently feeling irritated or agitated
- Too much weight gain or loss within a short period of time
- Sleeping too little or too much
- Low levels of energy or fatigue
- Poor self-esteem
- Concentration problems
- Reduced sex drive
- Increased thoughts of death and dying suicidal tendency
The symptoms mentioned above must have occurred during or after a specific substance/medication was taken or during withdrawal.
Committed to helping
people who want to help themselves
How Soon After Taking the Drug Can Depression Be Induced?
In some cases, symptoms appear almost straight away. There is even a category named “with onset during intoxication,” which means that the depressive episode actually begins when the individual is highly contaminated with the drug. It can also occur during withdrawal, during which symptoms of depression are commonly observed. Nevertheless, with depression which is simply a symptom of withdrawal, the person’s mood will usually get better within a few days of ceasing to take the drug, while with the substance-induced depression, it can begin during withdrawal, and continue or get worse as the person moves through the detox/treatment process.
Which Drugs Cause Substance/Medication-Induced Depressive Disorder?
A wide variety of addictive substances can cause substance-induced depression. The following disorders are recognized with the consumption of drugs given below:
- Unknown substance-induced depressive disorder
- Phencyclidine-induced depressive disorder
- Alcohol-induced depressive disorder
- Other hallucinogen-induced depressive disorder
- Opioid-induced depressive disorder
- Inhalant-induced depressive disorder
- Sedative-induced depressive disorder
- Anxiolytic-induced depressive disorder
- Hypnotic-induced depressive disorder
- Amphetamine-induced depressive disorder
- Cocaine-induced depressive disorder
- Other stimulant-induced depressive disorder
- Other substance-induced depressive disorder
Many medications are known to cause substance-induced depression. The following disorders are usually seen to be occurring due to the excessive consumption of the given medicines
• Immunological agent-induced depressive disorder
• L-dopa-induced depressive disorder
• Steroid-induced depressive disorder
• Antibiotic-induced depressive disorder
• Dermatological agent-induced depressive disorder
• Central nervous system drug-induced depressive disorder
• Chemotherapeutic drug-induced depressive disorder
Specific medications that have been caught up in medication-induced depression through investigation studies, retrospective observational studies, or case studies, which are prone to difficulty in determining the actual cause, include the following:
- Smoking cessation agents (varenicline), and immunological agents (interferon)
- Cardiovascular agents (such as clonidine, guanethidine, methyldopa, reserpine)
- Antiviral agents (such as efavirenz)
- Retinoic acid derivatives (such as isotretinoin)
- Antipsychotics
- Hormonal agents (corticosteroids, oral contraceptives)
- Antidepressants, anticonvulsants, anti-migraine agents (triptans)
- Gonadotropin-releasing hormone agonists, tamoxifen)
Committed to helping
people who want to help themselves
Causes of SIMD:
Substance / medication-induced depressive disorder is caused directly due to a specific substance/medication that is being consumed or during withdrawal from it. There are a number of substances and medications that could cause this, including:
- Alcohol
- Inhalants
- Phencyclidine
- Hallucinogens
- Amphetamines
- Opioids
Diagnosis of Substance-Induced Mood Disorder
According to the Diagnostic and Statistical Manual for Mental Disorders (DSM)-5, several criteria need to be met to have a diagnosis of substance-induced mood disorder. Mental health professionals need to do a complete and thorough assessment to differentiate the symptoms from those of independent depressive episodes or an episode of depression caused by any other medical issue. It is critical to conduct a complete physical evaluation, as well as laboratory blood tests, to rule out other causes for the depressive symptoms.
Diagnostic Criteria
- Persistent, prominent, and noteworthy mood disturbance that first occurred after reducing the consumption or withdrawal from a substance capable of causing depressive symptoms and continues after the initial withdrawal period.
- Absence of evidence that the depressive episode is independent of the substance use or began before taking the medication.
Mental health professionals might ask for a complete psychiatric history of immediate family members. Having a close family history of depressive episodes increases the chance of the individual to suffer from depression, independent of the medication usage or withdrawal.
Treatment of Substance-Induced Mood Disorder
Treating substance induced mood disorders requires a mixed approach. For many people with substance-induced mood disorders, combining psychotherapy and drug therapy has been more effective than just one or the other.
- Cognitive-behavioral therapy (CBT) and motivational interviewing
- Motivational Enhancement Therapy (MET)
- A calm environment
- A benzodiazepine or antipsychotic
These are all first choices of treatment, however, in most substance-induced psychoses, ceasing the consumption of substance and giving a benzodiazepine or antipsychotic drug is effective and for psychosis due to dopamine-stimulating drugs such as amphetamine and an antipsychotic drug is most effective. Like all other mood disorders, communication and support are critical for effective treatment and recovery.
Over 50% of opioids containing medications are being prescribed to individuals having pre-existing depression and other mood disorders. All patients receiving opioid therapy should be made aware of the risks of those medicines and should be carefully monitored during and after treatment.